Artificial Intelligence (AI)
The Role of AI in Revenue Cycle Management (RCM) in Healthcare

Artificial intelligence (AI) is rapidly transforming revenue cycle management (RCM) by enabling healthcare organizations to streamline, automate, and enhance core financial workflows. At its core, AI leverages advanced algorithms and machine learning to reduce reliance on manual, time-intensive processes that are often prone to error. In doing so, it allows revenue cycle teams to redirect their efforts toward higher-value, strategic activities.
Beyond automation, AI offers the ability to analyze large and complex datasets at scale. This enables organizations to uncover actionable insights, optimize revenue capture, and improve overall cash flow performance.
A range of AI technologies—including machine learning, optical character recognition (OCR), large language models (LLMs), generative AI, and emerging agentic AI—can be applied across the revenue cycle. Each plays a distinct role in improving efficiency, accuracy, and decision-making. This paper outlines key use cases and demonstrates how the thoughtful deployment of AI can materially enhance RCM performance.
Artificial intelligence (AI) is rapidly transforming revenue cycle management (RCM) by enabling healthcare organizations to streamline, automate, and enhance core financial workflows. At its core, AI leverages advanced algorithms and machine learning to reduce reliance on manual, time-intensive processes that are often prone to error. In doing so, it allows revenue cycle teams to redirect their efforts toward higher-value, strategic activities.
Beyond automation, AI offers the ability to analyze large and complex datasets at scale. This enables organizations to uncover actionable insights, optimize revenue capture, and improve overall cash flow performance.
A range of AI technologies—including machine learning, optical character recognition (OCR), large language models (LLMs), generative AI, and emerging agentic AI—can be applied across the revenue cycle. Each plays a distinct role in improving efficiency, accuracy, and decision-making. This paper outlines key use cases and demonstrates how the thoughtful deployment of AI can materially enhance RCM performance.
How AI is Used in Revenue Cycle Management
Healthcare providers are increasingly leveraging AI to automate processes, improve accuracy, and enhance workforce productivity across the revenue cycle. Common applications include eligibility verification, patient engagement, claims processing, compliance monitoring, and fraud detection.
AI-driven analytics further support financial performance by enabling organizations to forecast revenue, predict payment behavior, and proactively reduce claim denials. These capabilities allow teams to move from reactive to predictive revenue cycle management.
By automating repetitive and time-consuming tasks, AI enables staff to focus on more complex and strategic responsibilities, such as resolving high-value claims, improving patient financial experiences, and negotiating with payers. The result is a more efficient and resilient RCM function that integrates human expertise with technological precision.
The growing interest in AI is also driven by broader industry challenges, including workforce shortages, rising costs of care, declining reimbursement rates, and increasing pressure to reduce administrative expenses. AI presents a viable pathway to address these structural issues while improving operational outcomes.
What is Revenue Cycle Management (RCM)?
Revenue Cycle Management (RCM) is the process businesses—most commonly in healthcare—use to track and manage the financial flow from the moment a service is provided to when payment is fully collected.
At its core, it connects clinical/operational work to actual revenue.
The Full Revenue Cycle (Simple Breakdown)
- Patient Registration / Customer Intake
Collect basic info (name, insurance, demographics). - Insurance Verification & Eligibility
Confirm coverage and what’s billable. - Coding & Charge Capture
Translate services into standardized billing codes. - Claim Submission
Send the bill to the insurance company (or payer). - Adjudication (Processing by Payer)
Insurance decides what they’ll pay vs. what they won’t. - Payment Posting
Payments are recorded in the system. - Denial Management
Fix and resubmit rejected claims. - Patient Billing & Collections
Bill the patient for remaining balances and collect payment.
The Emergence of Agentic AI in RCM
While traditional AI tools have delivered incremental improvements, the emergence of agentic AI represents a step-change in capability. Unlike earlier solutions that rely heavily on human oversight or provide decision support, agentic AI systems can autonomously execute tasks, interact across systems, and manage workflows end-to-end.
This capability is particularly valuable in high-volume, rules-driven areas of the revenue cycle, such as patient billing inquiries, insurance verification, and payment follow-ups. By autonomously managing these processes, agentic AI can significantly reduce administrative burden, accelerate cycle times, and deliver measurable return on investment.
As a result, agentic AI is becoming a focal point for RCM leaders seeking scalable, sustainable efficiency gains.

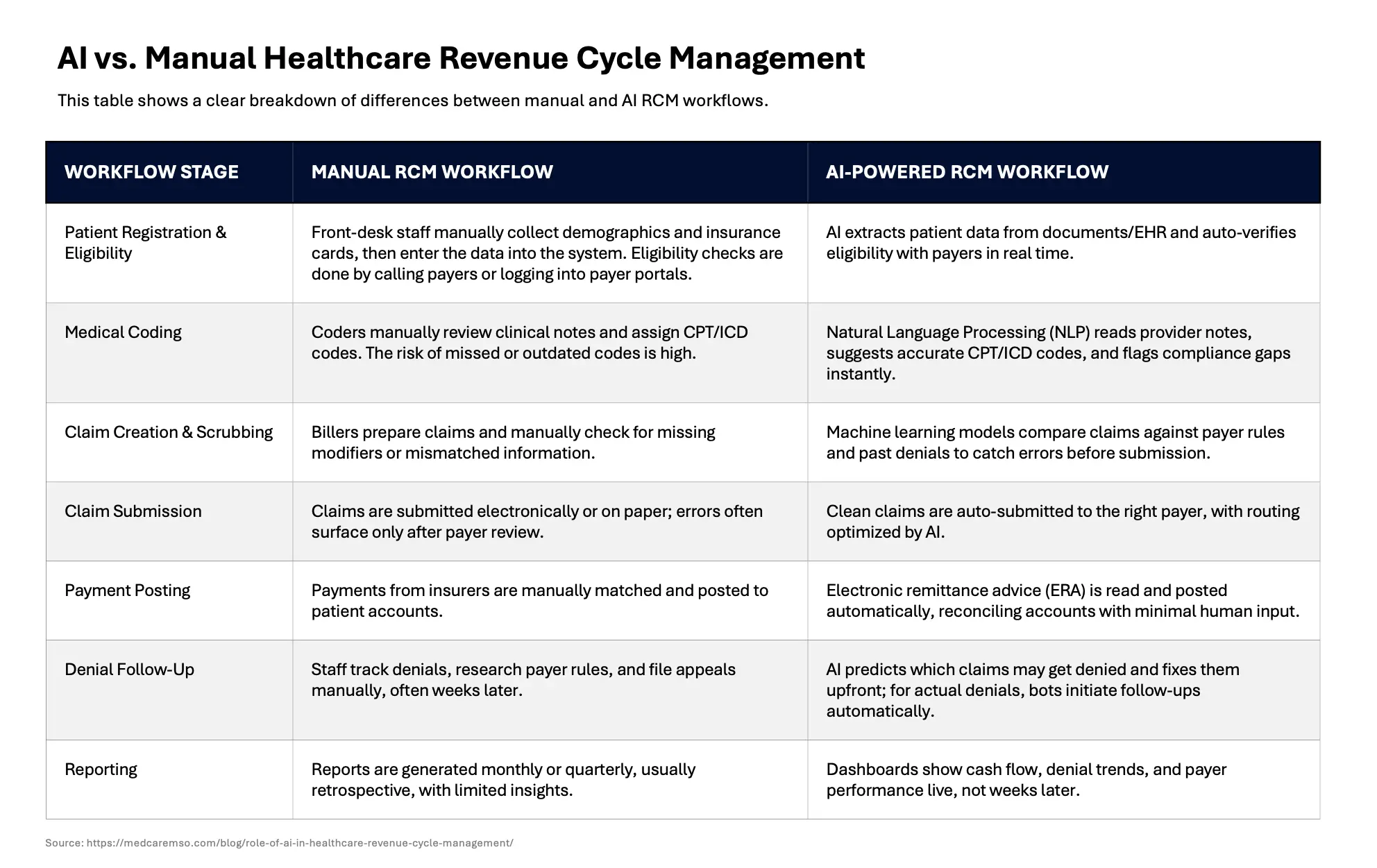
Automation vs. AI in RCM
Traditional revenue cycle automation focuses on executing predefined, rule-based tasks with minimal human intervention. Technologies such as robotic process automation (RPA) are well-suited for structured activities like data entry, eligibility checks, and claim scrubbing. These solutions have already demonstrated significant cost-saving potential across the healthcare system.
However, many RCM processes—such as denial management—are inherently complex and cannot be fully addressed through static rules alone.
AI extends beyond automation by introducing learning, adaptability, and decision-making capabilities. AI systems can continuously analyze data, identify patterns, and adjust their behavior over time without explicit programming. This enables them to handle more nuanced and dynamic workflows.
For example, while automation can reduce data entry errors through predefined validations, AI can proactively identify claims at risk of denial and recommend corrective actions before submission. Together, automation and AI create a more intelligent and proactive revenue cycle function.
Strategic Objectives of AI in RCM
In an environment characterized by rising costs and declining reimbursements, healthcare organizations are prioritizing efficiency, accuracy, and financial performance. AI supports these objectives across several dimensions:
- Revenue acceleration: Enhancing payer and patient collections through automated follow-ups, intelligent workflows, and personalized billing strategies
- Cash flow optimization: Reducing days in accounts receivable (A/R), improving point-of-service collections, and minimizing missed charges
- Data-driven decision-making: Leveraging predictive analytics to identify revenue leakage and optimize financial performance in real time
- Operational efficiency: Streamlining administrative processes such as insurance verification and financial data review
- Workforce enablement: Reducing manual workload and burnout while enabling staff to focus on higher-value activities
- Patient experience improvement: Simplifying billing, increasing transparency, and offering flexible payment options
- Accuracy and compliance: Reducing errors, improving claim quality, and strengthening fraud detection and regulatory adherence
- Enhanced oversight: Enabling real-time monitoring of key performance indicators and faster identification of anomalies
AI has the potential to significantly reduce administrative costs across the healthcare system, with estimates suggesting savings of up to $175 billion annually.
Key AI Technologies Used in Revenue Cycle Management
Healthcare organizations use a suite of AI technologies to enhance RCM. These include automation, machine learning, document processing, and intelligent agents.
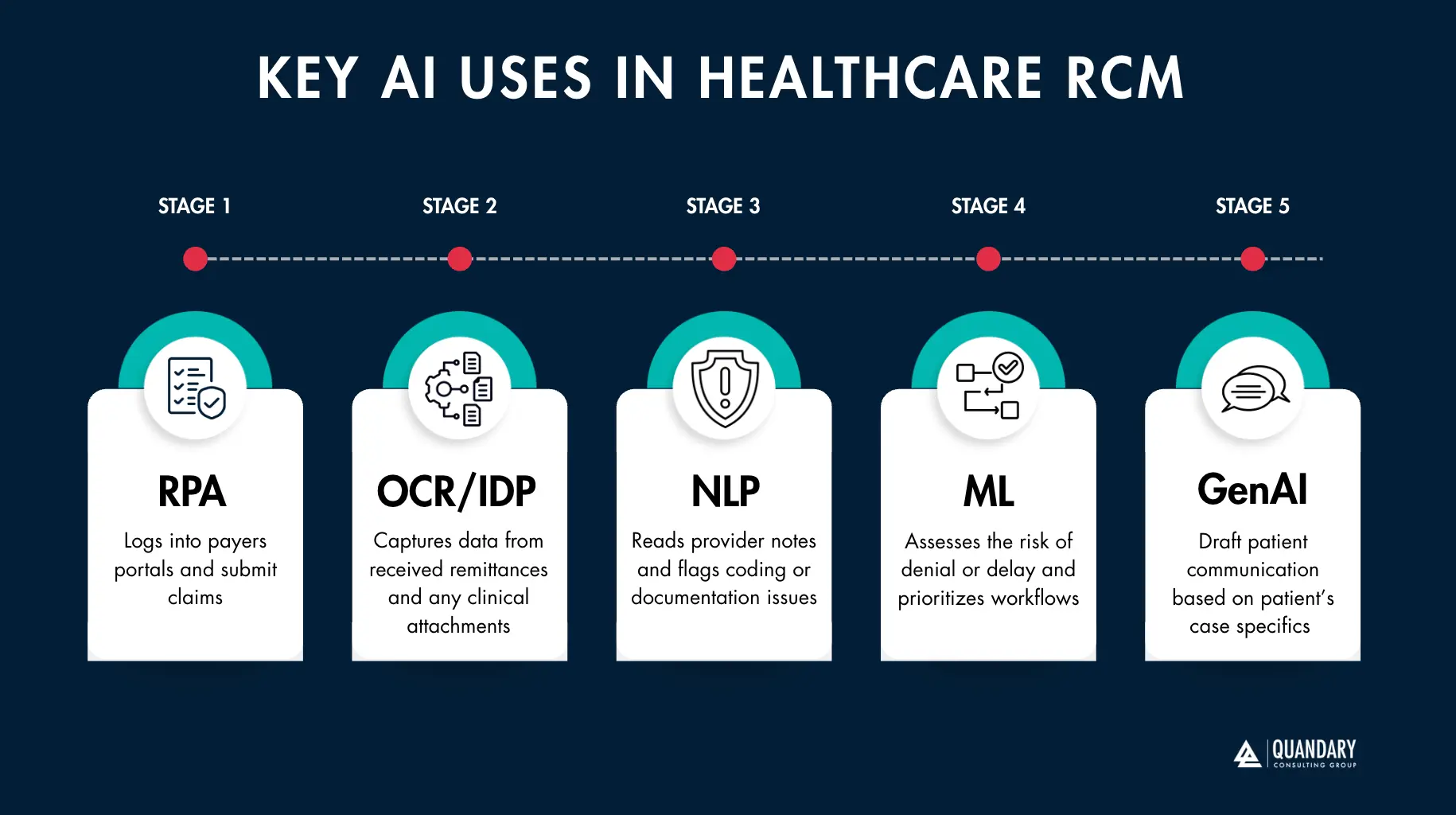
- One key component of AI in RCM is Robotic Process Automation (RPA). RPA uses software bots to copy data, enter information into portals, or click through workflows. It handles repetitive tasks and keeps them fast and consistent.
- Machine Learning (ML) adds prediction. It looks at past data to spot likely denials, underpayments, or patients who may not pay. This helps staff focus on targeting problems even before they arise.
- Natural Language Processing (NLP) reads notes, charts, and documents. It pulls out key details like diagnoses and procedures to support coding and documentation.
- Optical Character Recognition (OCR) and Intelligent Document Processing (IDP) turn messy files into usable data. They work on PDFs, faxes, and images. These tools pull patient and claim details from EOBs, referral letters, and other documents.
- Generative AI (GenAI) helps write foundational text. It generates appeal letters, prior authorization narratives, and patient communications. Human reviewers check and approve the content before it’s submitted.
Modern RCM uses a combination of these AI technologies to reduce manual effort and increase accuracy. The technologies work together, creating smarter, faster, and more adaptable revenue workflows that speeds up payment and improves the overall patient experience.
Regulatory and Industry Changes Driving AI Adoption
New rules are shaping how healthcare uses AI in revenue cycle management. Here are the key updates:
- CMS Interoperability & Prior Authorization (CMS-0057-F):
- Payers must implement FHIR‑based Patient and Provider Access APIs that include prior authorization data (excluding drugs), with full compliance by January 1, 2027; Some operational requirements begin in 2026.
- Medicare Pilot (WISeR Model):
- Starting January 2026, CMS will run the WISeR model in Arizona, New Jersey, Ohio, Oklahoma, Texas, and Washington, using AI tools plus clinician oversight to expedite prior authorization decisions on select procedures.
- Starting January 2026, CMS will run the WISeR model in Arizona, New Jersey, Ohio, Oklahoma, Texas, and Washington, using AI tools plus clinician oversight to expedite prior authorization decisions on select procedures.
- Federal Oversight:
- A 2023 Executive Order directed HHS to create an AI assurance policy for healthcare, setting expectations for safe and responsible AI deployment.
To learn more about this ruling, please visit Centers for Medicare & Medicaid Services (CMS.gov) CMS Interoperability and
Prior Authorization Final Rule (CMS-0057-F)

Key Applications of AI Across the Revenue Cycle
AI is increasingly embedded across every stage of the revenue cycle, from patient access through final payment. Common applications include:
Patient Billing Accuracy
AI improves billing accuracy by automating workflows such as eligibility verification, prior authorization, and payment posting. It reduces errors, enhances charge capture, and enables real-time monitoring of billing performance. Additionally, AI can identify patterns in denials and recommend corrective actions to prevent recurrence.
Medical Coding Efficiency
AI-powered coding solutions analyze clinical documentation to recommend accurate codes and identify missed charges. These tools improve coding consistency, increase productivity, and enhance key metrics such as clean claim rates and days in A/R. They can also support workforce training by providing real-time feedback and education.
Patient Payment Estimation
By analyzing historical and real-time data, AI enables more accurate patient payment predictions. It can identify patients at risk of non-payment and recommend tailored financial solutions, improving both patient satisfaction and revenue realization.
Benefits Verification and Prior Authorization
AI enhances data accuracy and reduces administrative friction by automating insurance verification and prior authorization processes. These tools help ensure that coverage details, deductibles, and copayments are accurate and accessible to both staff and patients.
Patient Billing Support
AI-powered chatbots and virtual agents extend support capabilities beyond traditional hours, providing real-time assistance to patients. Advanced AI agents can resolve inquiries, collect payments, and even establish personalized payment plans with minimal human intervention.
Personalized Patient Communications
AI enables targeted, timely communication with patients, including appointment reminders, payment notifications, and cost estimates. These capabilities improve transparency, increase engagement, and reduce confusion around healthcare costs.
Claims Processing
AI streamlines claims submission and management by identifying errors, tracking claim status, and predicting denial risk. OCR and automation technologies further reduce manual workload by digitizing and standardizing claim data.
RCM Operations and Workforce Enablement
AI also supports internal operations by improving training, performance management, and decision-making. For example, AI-driven tools can help standardize best practices and elevate the performance of less experienced staff.

The Future of AI in Revenue Cycle Management
Adoption of AI in RCM is accelerating, with a majority of healthcare organizations actively evaluating new technologies. While the potential benefits are substantial, successful implementation requires a disciplined approach, including strong governance, integration with existing systems, and ongoing oversight.
When deployed effectively, AI has the potential to fundamentally transform revenue cycle operations—delivering improved financial performance, enhanced patient experiences, and more sustainable workforce models.
How Quandary Can Help
Realizing the full value of AI in revenue cycle management requires more than technology—it demands a clear strategy, thoughtful implementation, and ongoing optimization. Many organizations struggle not with identifying opportunities, but with operationalizing them in a way that delivers measurable and sustainable results.
Quandary partners with healthcare organizations to bridge this gap. By combining deep revenue cycle expertise with a pragmatic approach to digital transformation, Quandary helps clients identify high-impact use cases, select and implement the right technologies, and redesign workflows to maximize efficiency and performance.
From initial assessment through implementation and continuous improvement, Quandary works alongside your team to ensure AI initiatives are aligned to your strategic priorities, integrated seamlessly into your existing ecosystem, and positioned to deliver tangible ROI.
Whether you are beginning to explore AI or looking to scale existing capabilities, Quandary provides the guidance and execution support needed to modernize your revenue cycle and unlock meaningful financial and operational value